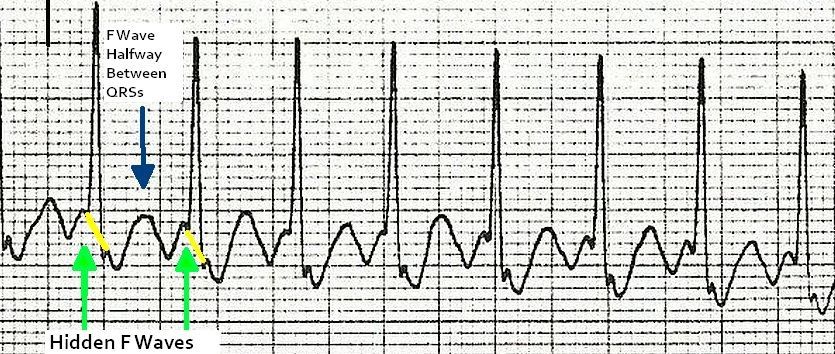
If there is 1:1 conduction, the ventricular rates will be very high. If the waves are positive in inferior leads, it is clockwise loop and if negative, the re-entry loop is counter-clockwise.Ītrial flutter is usually associated with a fixed ratio AV block. The direction of the less sharp component of the flutter wave is taken as the direction of the wave. Isthmus dependent flutter can be typical and reverse typical depending on whether the re-entry is counter-clockwise or clockwise. Non isthmus dependent flutters are the scar related flutters and caval mediated flutters. In the left atrium there is mitral isthmus. In the right atrium it is the cavotricuspid isthmus. Atrial flutter can be classified into isthmus dependent and non-isthmus dependent. It may convert into atrial fibrillation over time or, after administration of drugs such as digoxin.Atrial flutter is an organized atrial tachyarrhythmia due to macro re-entry typically with saw tooth shaped flutter waves in the ECG. The causes of atrial flutter are similar to those of atrial fibrillation, although idiopathic atrial flutter is uncommon. Manoeuvres that induce transient atrioventricular block may allow identification of flutter waves. The non-conducting flutter waves are often mistaken for or merged with T waves and become apparent only if the block is increased. Identification of a regular tachycardia with this rate should prompt the diagnosis of atrial flutter. Typically 2:1 block (atrial rate to ventricular rate) occurs, giving a ventricular rate of 150 beats/min. 
The ventricular rate depends on conduction through the atrioventricular node. These are broad and appear saw-toothed and are best seen in the inferior leads and in lead V1. This produces atrial contractions at a rate of about 300 beats/min-seen on the electrocardiogram as flutter (F) waves. It may be precipitated by an atrial extrasystole or result from degeneration of other supraventricular tachycardias, particularly atrial tachycardia and/or flutter.Ītrial flutter is due to a re-entry circuit in the right atrium with secondary activation of the left atrium. Mapping R waves against a piece of paper or with calipers usually confirms the diagnosis.Ītrial fibrillation may be paroxysmal, persistent, or permanent. The RR interval remains irregular, however, and the overall rate often fluctuates. Slower rates suggest a higher degree of atrioventricular block or the patient may be taking medication such as digoxin.įast atrial fibrillation may be difficult to distinguish from other tachycardias. The ventricular rate depends on the degree of atrioventricular conduction, and with normal conduction it varies between 100 and 180 beats/min. This combination of absent P waves, fine baseline f wave oscillations, and irregular ventricular complexes is characteristic of atrial fibrillation. Only a few of the impulses transmit through the atrioventricular node to produce an irregular ventricular response. The amplitude of these waves varies between leads but may be so coarse that they are mistaken for flutter waves.Ĭonduction of atrial impulses to the ventricles is variable and unpredictable. 
Atrial fibrillation is seen on the electrocardiogram as a wavy, irregular baseline made up of f (fibrillation) waves discharging at a frequency of 350 to 600 beats/min. These are often triggered by rapid firing foci. 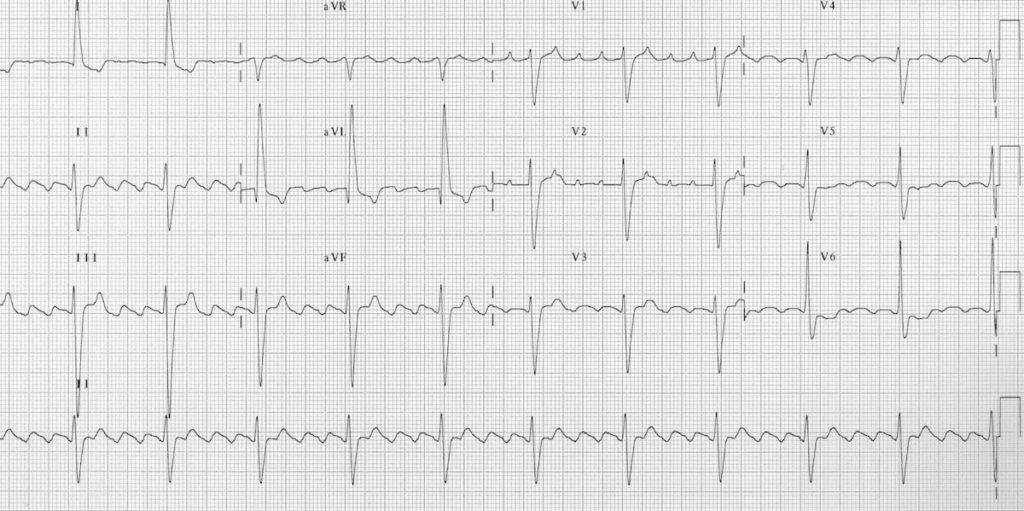
Prognosis is related to the underlying cause it is excellent when due to idiopathic atrial fibrillation and relatively poor when due to ischaemic cardiomyopathy.Ītrial fibrillation is caused by multiple re-entrant circuits or “wavelets” of activation sweeping around the atrial myocardium. Causes are varied, although many cases are idiopathic. Overall prevalence is 1% to 1.5%, but prevalence increases with age, affecting about 10% of people aged over 70. This is the most common sustained arrhythmia.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
